Our Products
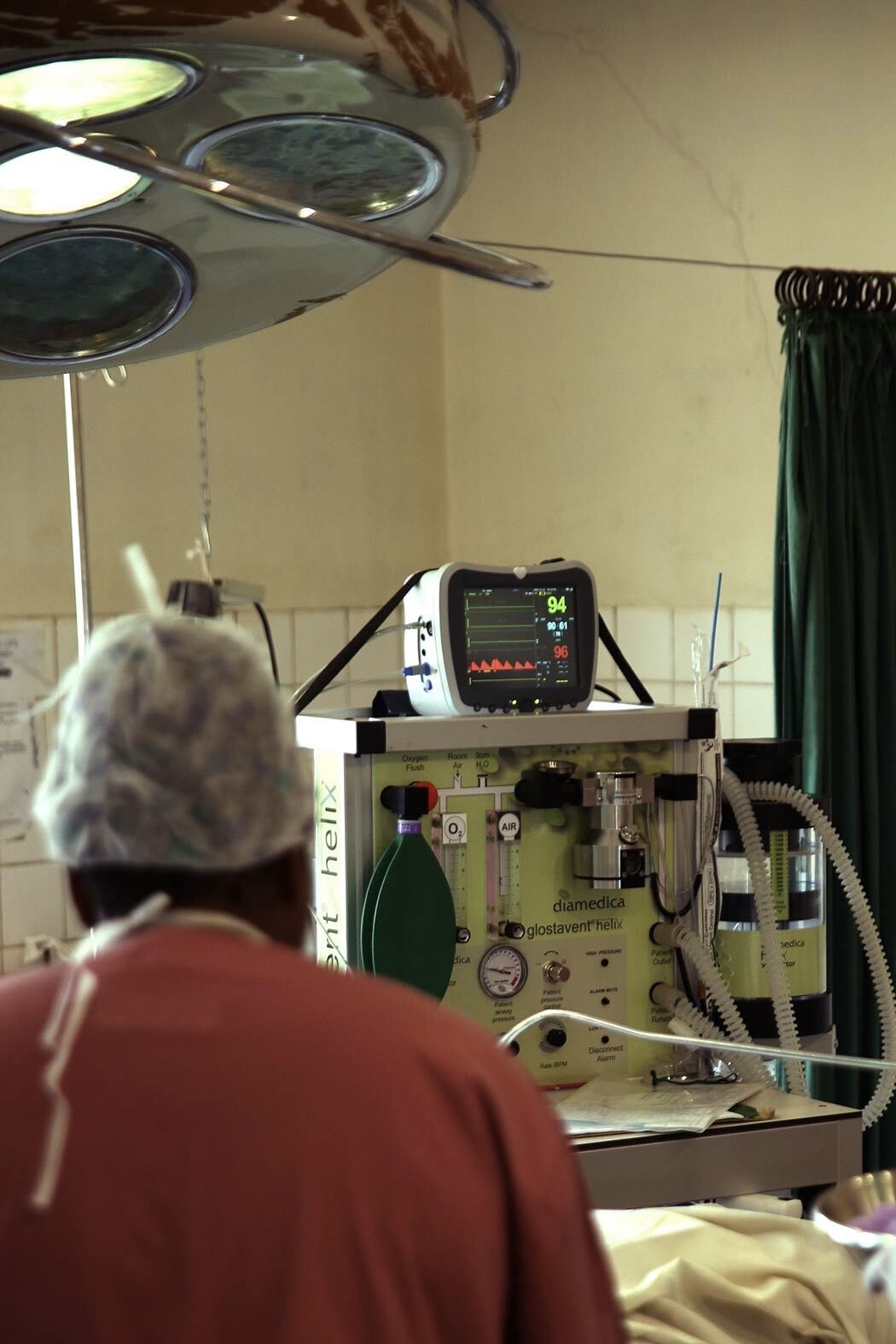
Anaesthesia
Anaesthesia systems for limited resource environments
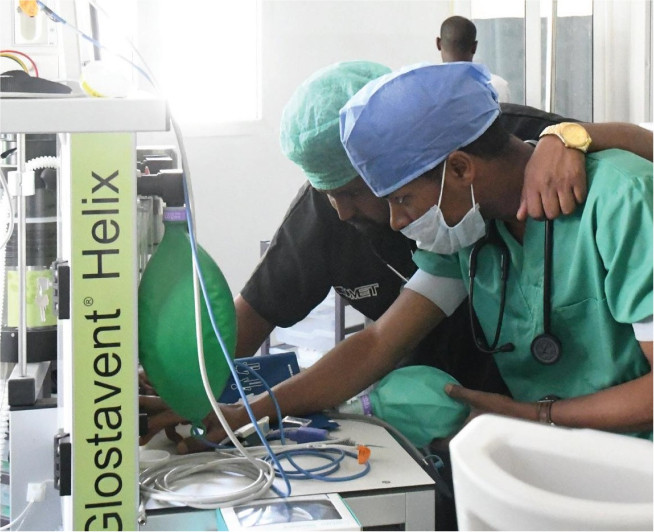
Intensive Care and Pain Management
A versatile ventilation system assisting breathing around the world
Oxygen Therapy Equipment
An inexpensive and efficient source of oxygen
Neonatal Care
Life-saving respiratory and resuscitation solutions for preterm babies
Monitoring
A perfect fit for monitoring your anaesthesia machine
Surgical Accessories
Affordable and essential surgical accessories for improved medical outcomes
Latest News
Find out about our latest news updates.